Hantavirus is back in the news. A cruise ship outbreak in the Atlantic has killed three people, hospitalized passengers across at least seven countries, and triggered an international public health response that involved evacuating Americans on a U.S. government medical flight to a quarantine center in Nebraska. Yet most people couldn’t tell you what hantavirus actually is, where it comes from, or what to do if they think they’ve been exposed.
This is a guide to all of that — written for people who don’t have a medical degree.
What is hantavirus?
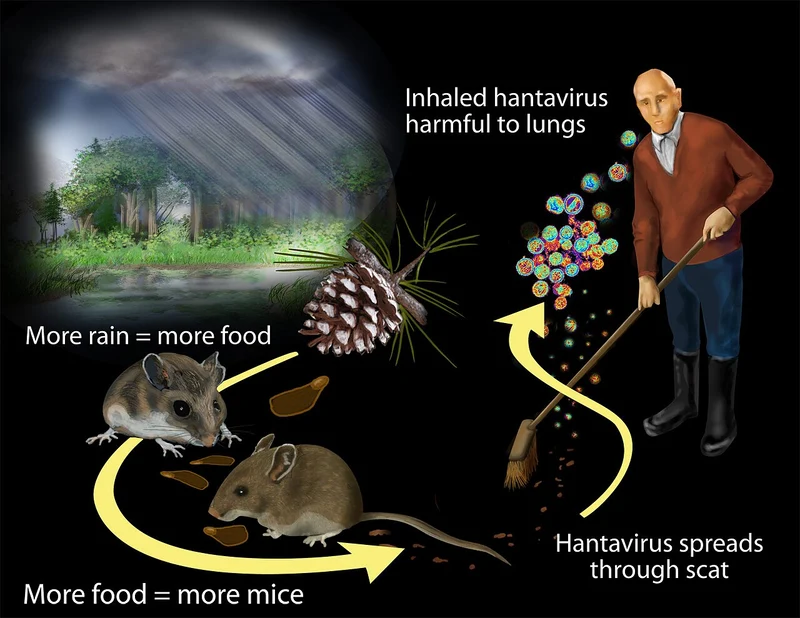
Hantavirus is not a single virus. It’s a family of more than fifty related viruses, each carried by a specific kind of rodent — most often deer mice, cotton rats, rice rats, white-footed mice, and a few species of South American mice. The rodents themselves don’t get sick. They carry the virus quietly for their whole lives and shed it in their urine, droppings, and saliva.
When a human breathes in, swallows, or otherwise picks up the virus from those rodent excretions, the results can range from a bad flu-like illness to a rapid, life-threatening medical emergency.
There are two main forms of serious hantavirus disease:
Hantavirus Pulmonary Syndrome (HPS) — Found in the Americas. Attacks the lungs and heart. The U.S. Centers for Disease Control and Prevention reports that about 38 percent of people who develop the full respiratory form of the illness die from it.
Hemorrhagic Fever with Renal Syndrome (HFRS) — Found mostly in Europe and Asia. Attacks the kidneys. Depending on the strain, fatality rates range from less than 1 percent to as high as 15 percent.
The strain getting attention right now is the Andes virus, a South American hantavirus that causes HPS and has one frightening trait the others don’t: it can spread from person to person.
How do people get it?
In the vast majority of cases, hantavirus infection happens because someone breathes in tiny airborne particles from dried rodent urine, droppings, or nesting material. The classic scenario is sweeping out a shed, cabin, garage, barn, or basement that mice have moved into. The act of sweeping or vacuuming kicks the contaminated dust into the air, and the person inhales it without realizing what they’ve done.
People can also catch it by:
- Touching surfaces contaminated with rodent waste and then touching their eyes, nose, or mouth
- Eating food that has been contaminated by mice
- Being bitten or scratched by an infected rodent
You cannot get hantavirus from mosquitoes, ticks, dogs, cats, or other pets. With one exception — the Andes virus — you also cannot catch it from another person. Casual contact with someone who has HPS in the United States poses no risk.
The Andes virus is the outlier. It has been documented spreading between people through close, prolonged contact — sharing a small living space, sustained exposure to a sick person’s saliva or respiratory droplets, caring for someone without protection. It does not appear to spread through brief, casual contact, and public health experts have emphasized that it lacks the explosive transmission profile of a virus like COVID-19.
A professor of exposure assessment science at Harvard University appeared on MS NOW to voice concerns about the information coming from our government and public health officials. Professor Joseph G. Allen claimed that he had spoken with a doctor treating passengers on the cruise ship where the outbreak occurred.
He stated that the doctor had shared information with him regarding the conditions under which hantavirus spreads from person to person. What the doctor shared was different from the details being shared with the public.
The media and public health officials were reporting that the virus spread from person to person with prolonged, close contact only. However, the cruise ship physician told Professor Allen that he had observed people getting infected after being in a room where an infected passenger had previously been.
He also referenced a case of a passenger getting sick after briefly walking past an infected passenger.
I am NOT a medical professional.
Please contact your family physician with any questions or concerns you have about this virus. This explainer highlights information as it is currently being shared by the CDC. We want our readers to have as much detailed information as possible so they can take proper precautions. That’s why Professor Allen’s statements are included.
We will update this article if any of the information coming from the CDC changes.
What are the symptoms of hantavirus?
Symptoms of hantavirus pulmonary syndrome typically begin one to eight weeks after exposure, with most cases showing up around two to three weeks in.
The illness moves through distinct phases.
The early phase lasts a few days and looks almost exactly like the flu: fever, chills, deep muscle aches (especially in the thighs, hips, and back), headache, fatigue, dizziness, nausea, vomiting, diarrhea, and abdominal pain. This is the most dangerous window for misdiagnosis. People often assume they have a stomach bug or the flu and stay home.
The cardiopulmonary phase is when things turn serious, often within a day or two of the first symptoms getting worse. The capillaries in the lungs begin to leak. Fluid fills the lungs. Breathing becomes difficult. The heart races, blood pressure crashes, and patients can deteriorate from “uncomfortable” to “critical” within hours.
Without aggressive supportive care, most deaths happen within 24 to 48 hours of this phase starting.
The recovery phase, for those who survive, this phase can last weeks to months. Some people experience lingering shortness of breath for up to two years.
The kidney form of the disease, HFRS, follows a different path — sudden fever, back pain, abdominal pain, blurred vision, flushing of the face, and eventually low blood pressure and kidney failure that may require dialysis.
How is it treated?
This is the hard part: there is no specific antiviral drug for hantavirus. There is no vaccine approved in the United States.
Treatment is what doctors call “supportive care,” which means treating the symptoms aggressively and giving the body time to fight the virus itself. For severe cases, that includes oxygen, mechanical ventilation (ventilator), careful fluid management, and medications to support blood pressure.
In the worst cases, a machine called ECMO (extracorporeal membrane oxygenation) can take over the work of the lungs and heart (you probably heard about this during the COVID pandemic).
CDC guidance notes that early ECMO can push survival as high as around 80 percent in severe HPS — but only when it’s started in time.
The single most important factor in surviving hantavirus is early recognition. If you have been around rodents or rodent droppings in the past several weeks and you develop flu-like symptoms, tell your doctor about the exposure right away.
Do not wait to see if it gets better. The early window is when treatment decisions matter most.
Who is most at risk?
Hantavirus is rare. Since surveillance began in the U.S. in 1993, the CDC has counted fewer than 900 cases through 2023. But certain people face higher exposure:
- Anyone cleaning out cabins, sheds, barns, garages, or vacation homes that have been closed up
- Farmers, ranchers, and agricultural workers
- Construction, utility, and pest control workers
- Hikers and campers using rural cabins
- People living in rural areas of the western United States, where deer mice are widespread
- People living in housing with active rodent infestations
In the U.S., hantavirus cases cluster heavily west of the Mississippi River, with the Four Corners region historically the epicenter. It was here, in 1993, that doctors first identified the disease during a mysterious outbreak that killed previously healthy young adults.
How can I protect myself?
The single best protection is keeping rodents out of the spaces where you live, work, and sleep — and cleaning up any signs of them safely.
Seal them out. Mice can squeeze through holes as small as a quarter-inch wide. Use steel wool, metal flashing, or cement to close gaps around pipes, vents, doors, foundations, and rooflines.
Take away the food and the shelter. Store food, pet food, and birdseed in rodent-proof containers. Wash dishes promptly. Use tight-fitting lids on trash cans. Clear brush, woodpiles, and junk away from your home’s foundation.
Set traps. Spring-loaded snap traps along baseboards remain the standard recommendation.
Clean carefully — this part matters. Never sweep or vacuum droppings, nests, or dead mice. Sweeping launches the virus into the air, which is exactly how people get sick. The CDC’s safer method:
- Open windows and doors to air out the space for at least 30 minutes before you start, and leave them open while you work.
- Wear rubber, latex, or vinyl gloves.
- Spray droppings, nests, and dead rodents thoroughly with a disinfectant or a bleach solution (one part bleach to ten parts water) and let it soak for at least five minutes.
- Use paper towels to pick everything up, then place it in a sealed plastic bag, then a second sealed bag, then the outdoor trash.
- Disinfect the area again afterward, including any surfaces nearby.
- Wash your hands thoroughly with soap and warm water.
For heavily infested spaces, a respirator with N100 or HEPA filtration is recommended, along with goggles and a coverall.
Why the cruise ship outbreak matters — and why it probably won’t become the next pandemic
The current outbreak aboard the MV Hondius, a Dutch cruise ship that became the focus of an international evacuation operation, involves the Andes strain — the only hantavirus known to spread between people.
As of mid-May 2026, there have been nine confirmed cases, two probable cases, and three deaths linked to the ship, with patients spread across hospitals in South Africa, the Netherlands, Germany, Saint Helena, Spain, France, and Switzerland.
Eighteen American passengers were flown to a quarantine center in Nebraska for monitoring.
This sounds alarming, and for the people directly affected, it is. But the World Health Organization and the European Centre for Disease Prevention and Control have both classified the broader public risk as very low. Andes virus spreads through close, sustained contact — not through the kind of brief encounters that allow respiratory viruses like influenza or COVID-19 to circle the globe in weeks.
Every previous outbreak of person-to-person Andes virus transmission has been small and contained, and there is no indication this one will behave differently once exposed passengers complete their quarantine.
The lesson of this outbreak is less “panic about a new pandemic” and more “take rodent contact seriously, especially when traveling in regions where these viruses are endemic, and pay attention when flu-like symptoms follow that contact.”
Hantavirus is rare, but it is unforgiving when it strikes. Most people who get sick from it could have avoided it with a pair of gloves, a spray bottle of bleach solution, and the knowledge that they shouldn’t have grabbed the broom.










